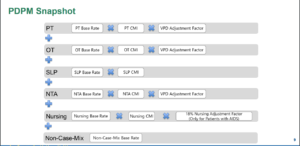
As of October 1, 2019, Medicare is shifting nursing home reimbursement from the "Resource Utilization Group" methodology to the Patient Driven Payment Model or "PDPM." Rather than current model which is driven by the hours of therapy minutes billed, the new driver will be case mix indexes or "CMIs."
The new model looks like this:
The Case Mix Index or "CMI" for each of the components is determined by coding. There is a complicated crosswalk of diagnosis codes for each of the CMIs above. Since almost all nursing homes currently rely on their MDS vendor software to provide coding, most nursing homes will initially rely on their software vendor for the coding driving PDPM reimbursement. The majority of nursing home MDS Directors do not understand the underlying codes generated by their software. They never had to in the past.
In helping nursing homes get ready for October 1, 2019, we look at their last year of billed claims using our parsing software and the nursing home's electronic billing data.
We perform an initial analytical review of the overall data. We compare data at the patient level to the MDS data looking for potential coding issues. Finally we get down into the weeds and review coding for individual patients. We do all this to help nursing homes revise their billing and coding procedures to ensure proper coding that leads to proper reimbursement. As software vendors struggle with MDS, this may require that vendor billing output be modified before billings are submitted.
We know that nursing homes will be now forced to understand coding and MDS. We are there to help.
Timothy Powell, CPA CHCP